What is the Lymphatic System?
The lymphatic system is becoming increasingly more talked about but is still, in my opinion, one of the least appreciated and under-utilised systems in the restoration of movement dysfunctions and chronic health complaints.
Everybody, including health practitioners and those in the fitness industry, could benefit from understanding and implementing lymphatic techniques. You can consider that a homeostatic balance of the internal environment can be a true measure of health.
Lymphatic techniques can, therefore, aid the body in moving towards more of an internal state of homeostasis.
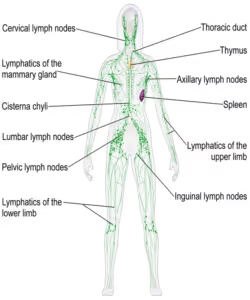
How does the lymphatic system function?
The lymphatic system is, in essence, the sewage system of the body.
It has the incredible ability to trap nearly all soluble antigens, roughly 99%, with its role in waste removal. This is significantly important for the other body systems to not become overwhelmed and develop issues as well.
The lymphatic system contains the thymus, an endocrine organ which is responsible for the development of T-lymphocytes, immune cells that are involved in fighting infection through the process of cell-mediated immunity.
The spleen plays a key role in the lymphatic system as the largest lymphatic organ, having a vital role in a host of detox processes, such as:
- Filtering blood
- Removing old dead red blood cells
- The maturation of lymphocytes and macrophages to aid in fighting infection
The splenic communication of the tenth cranial nerve, the Vagus nerve, is crucial in reducing inflammatory cytokine production.
The tonsils also form part of the structure of the lymphatic system. With the tonsils formed of lymphatic tissue, housing lymphocytes and macrophages, they protect the digestive system and lungs from pathogens entering through the nose or mouth.
There is also a deep association with the gastrointestinal system through gut associated lymphoid tissues (GALT) known as Peyers Patches, with the role of the gastrointestinal system intrinsically linked to the immune system. Estimates suggest that roughly 70-80% of immune function is beholden to gastrointestinal health.
This amazing system also comprises millions of lymphatic vessels which, if placed end to end in a continuous line, would circle the earth four times! Alongside these vessels there are over seven hundred lymph nodes within the body, with the most populated areas being the neck, skin and the intestines.
This mass of lymphatic vessels works in uniform direction towards the heart, with valves interspersed to prevent any backflow from occurring. This one-way system is aided by the structure of the vessels which allow fluids to flow in the direction of clearance, but with numerous valves preventing backflow. Allowing the system to be cleared, very much how a filtration device on a fish tank would work.
The ability to regulate fluid homeostasis is a key aspect of the lymphatic system. The body contains fifteen litres of lymphatic fluid, predominantly of water, and roughly 10% of proteins, hormones and waste products. Comparing this to the five litres of circulating blood that we have, the body wouldn’t contain three times more lymphatic fluid than blood if it wasn’t a critical component of our survival!
From the five litres of circulating blood, over the course of a day, three litres of plasma leaks out into the interstitial space.
If not appropriately removed through the lymphatic system this can lead to swelling outside of the cellular space due to the increased fluid concentration and alterations in pressure.
Without effective drainage this can create stagnation in the fluids;
Let’s go back to the fish tank analogy above, we know that stagnation of fluids is detrimental to the ecosystem, the same being the case for our health.
In a system with appropriately functioning lymphatics, this plasma is removed from the interstitial space into the lymphatics system and circulated upwards towards the subclavian vein. This is where it flows into the venous system, before returning to the liver, detoxifying and purifying the blood.
Taking a deeper look into the pathway of the lymphatic vessels will give an understanding into the application of treating the lymphatic system.
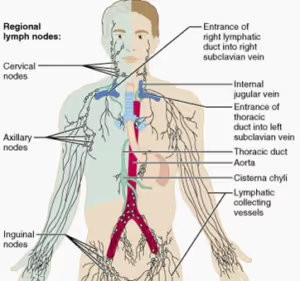
As a one way system drains into the venous system at the bilateral sites of the subclavian veins, all lymphatic vessels are required to flow in this direction. The right upper quadrant of the body drains through the right lymphatic duct and into the right subclavian vein, whilst the remainder of the body drains through the thoracic duct into the left subclavian vein.
The thoracic duct is responsible for the majority of lymphatic flow and also houses the largest lymph node, the cisterna chyli, which is a major site of drainage for the liver. It’s crucial to keep this node functioning well as between 25-50% of the returning lymphatic fluid through the thoracic duct is returned from the liver.
There is an important bidirectional relationship between the cisterna chyli and the liver, with an overburdened liver that can’t move or function optimally placing more load on the cisterna chyli. Having a lymphatic system that can’t drain well, especially at the cisterna chyli, increases the potential to create stagnation around the liver. A lymphatic vessel that is unable to drain will not be able to receive fresh supply creating this backlog.
A fairly recent discovery reveals that the lymphatic system also continues up into the central nervous system through the glymphatics, more commonly known as the glymphatic system.
The glymphatic system has the same role as the lymphatic system, however it is only situated in the brain. This helps to reduce inflammation and drive the removal of waste products which is essential for overall brain health. Additionally, the protective benefits of this system helps to distribute fuel sources and various other vital components around the brain.